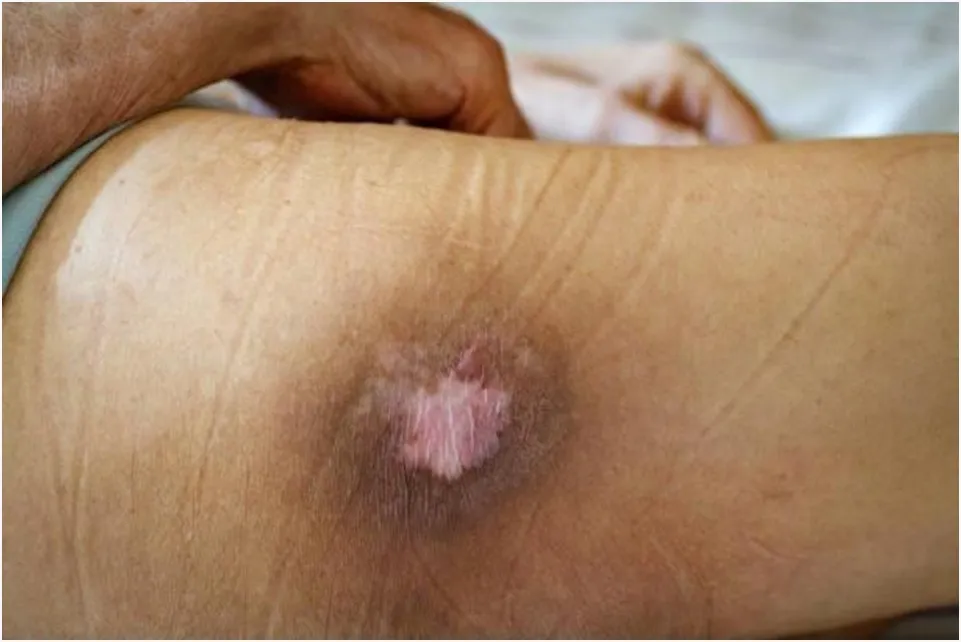
Are you suffering from bed sores?
Imagine sitting or lying in one position for too long. Your skin can break down, and that’s when bed sores happen. Bed sores are also known as pressure sores or pressure ulcers. They are skin wounds that develop when there’s prolonged pressure on one area of the body.
These sores can cause severe problems for patients. They can extend to deeper tissues they can even go up to muscles and bones. That’s why seeking help from experts like Dr. Leena Jain, a skilled plastic surgeon in Bandra, is crucial.
In this blog, we’ll delve into the world of bed sores, understand their impact on patients, and explore the effective solutions provided by Dr. Leena Jain and explore the effective solutions provided by Dr. Leena Jain, one of the best plastic surgeons in India to heal these sores and prevent them from recurring.
Signs and Symptoms of Bed Sores
Recognizing the signs and symptoms of bed sores is crucial for early intervention and effective treatment.
- The skin might look reddish, bluish, or purplish.
- Patient soften may not feel pain in the affected area as they are patients of stroke
- The skin can feel warmer than the surrounding areas.
- Swelling may occur around the sore.
- Bed sores might appear as open wounds or blisters.
- Some sores may ooze fluid.
- The skin can become rough or scaly.
- Tip of iceberg: they appear small on surface but are extensive inside
If you notice any of these signs or symptoms, please seek prompt medical attention from Dr. Leena Jain. A well-known plastic surgeon in Mumbai, she can provide expert care and treatment for bed sores.
Understanding the causes and risk factors behind bed sores is essential in preventing these skin wounds. So, let’s find out what can cause bed sores.
Causes and Risk Factors of Bed Sores

- Pressure: Sitting or lying in one position for a long time can press on the skin and cause bedsores.
- Friction: Rubbing the skin against bedding or clothing can damage skin especially while turning the patient, etc.
- Moisture: Damp skin from sweat or urine can make skin more vulnerable to bed sores.
- Limited Mobility: People who can’t move easily are at higher risk/due to lack of sensations and maceration.
- Poor Nutrition: Not getting enough protein and low haemoglobin will impact wound healing.
- Advanced Age: Older adults are more vulnerable to bed sores.
- Medical Conditions: Health issues like stroke, diabetes, circulation problems, or spinal cord injuries increase the risk.
- Thin Skin: Fragile or thin skin is more prone to bed sores.
- Smoking: Smoking reduces blood flow, affecting skin health.
“Bed sores can develop in areas where bones are close to the skin,” explains Dr. Leena Jain, known to many as the best plastic surgeon in Borivali. “Areas like heels, hips, lower back, and elbows are the most vulnerable. They can also appear on the back of the head if you lie on your back for too long.”
If you think you may be prone to bedsores, seek advice from Dr. Leena Jain, a specialist in pressure ulcer treatment.
Don’t wait! Care for early-stage bed sores can prevent them from getting worse.
Stages of Bed Sores
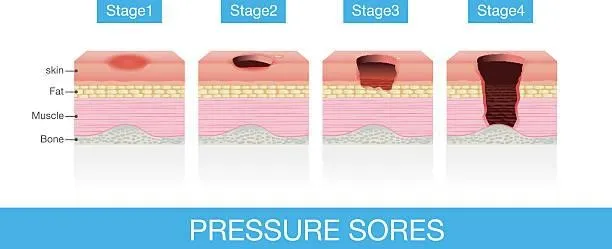
Stage 1 Pressure Ulcer: The skin is red but not broken in the early stage. It might be warm, macerated or itchy.
Stage 2 Pressure Ulcer: The skin breaks, forming a shallow sore like a blister or abrasion.
Stage 3 Pressure Ulcer: The sore gets deeper, reaching beneath the skin’s surface.
Stage 4 Pressure Ulcer: The wound is severe, affecting muscles, bones, and sometimes joints.
Are you or a loved one worried about bed sores? Consult Mumbai’s highly-skilled plastic surgeon, Dr. Leena Jain, for effective treatment and a speedy recovery.
Now, let’s talk about the Treatment Options for bed sores.
Bed Sores Treatment Options
Stage 1 Pressure Ulcers:

- Relieve pressure by changing positions regularly.
- Keep the area clean and dry.
- Use air mattresses/ special cushions or padding.
- Apply padding as a precaution to extension
Stage 2 Pressure Ulcers:
- Clean the wound gently and keep it covered.
- Apply prescribed dressings.
- Continue pressure relief techniques.
- Manage infection, if present
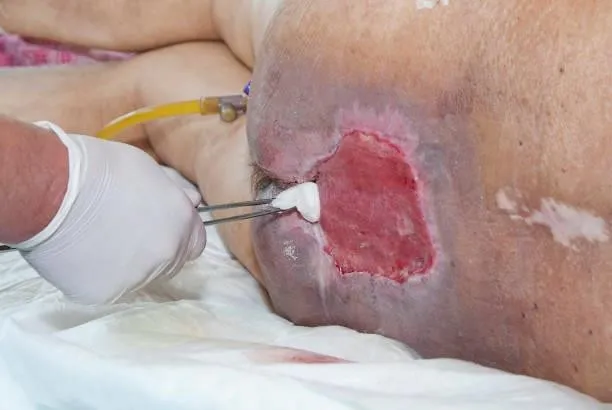
Stage 3 Pressure Ulcers:
- These will require debridement (removing dead tissue)/ black patches.
- More intensive wound care is needed.
- VAC dressing to facilitate healing and reduction in size of wound
- Will require Antibiotics if there’s an infection.
- Maintain pressure relief and repositioning.
Stage 4 Pressure Ulcers:
- Debridement and cleaning are essential
- Extensive wound care, often involving surgery.
- Surgery: use of flaps to cover the wound
- Rigorous infection control measures.
- Pressure relieving aids
- Nutrition: haemoglobin and protein deficiencies need to be corrected
Flap Surgery
Bed sores are best covered with flaps taken from the adjacent area. Flaps can be rotated or advanced into the defect to fill it. These are all designed based on their blood supply and planned in a way that in case a sore recurs, the same flap can be advanced to cover it up again. Anatomical knowledge and planning are essential for these flap surgeries which are the best to heal the wounds and prevent recurrence.
Have you noticed any signs of bed sores like red or broken skin or changes in skin texture? It’s crucial to seek help early.
Please consult a plastic and reconstructive micro surgeon like Dr. Leena Jain to determine the most suitable treatment plan.
Read on to understand why it is essential not to ignore a bedsore. Here, we list the complications and long-term effects of bed sores.
Complications of Bed sores
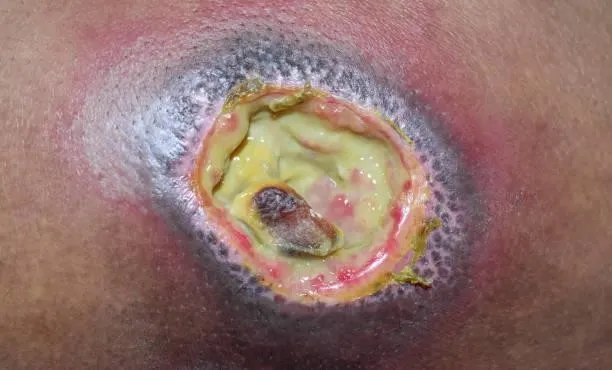
Bed sores can lead to serious problems, including:
- Infections: Open sores may get infected, causing significant health issues.
- Cellulitis: The skin can swell and become red and painful.
- Abscesses: Pus-filled pocket scan form under the skin.
- Sepsis: In severe cases, an infection can spread throughout the body.
Long-Term Effects:
- Scarring: Healed bed sores may leave scars.
- Extension of ulcers: often what is seen on the surface is only a tip of the iceberg; deep down they can extend and be infective.
- Chronic non healing ulcer: Sores may at times persist and be unrelenting
- Recurrence: Without proper care, bed sores may return or may come at other sites.
So, please do not take bed sores lightly. It’s crucial to prevent bedsores from worsening. Seek timely treatment to avoid these complications and long-term effects.
Conclusion

Bed sores can be chronic and extensive and can lead to infective complications. If you or a loved one is facing bed sores, seeking prompt treatment is vital. Dr. Leena Jain, a skilled plastic surgeon, can provide the treatment needed for a faster recovery and better quality of life. Treatment may include cleaning and dressing the wounds, relieving pressure and flap surgery to cover them.
With nearly 8 years of experience and countless happy patients, Dr. Jain is often called the best plastic surgeon in Bandra.
Don’t hesitate to contact Dr. Leena Jain today for the help you deserve. Your health and comfort matter.
FAQ
Q. What do bed sores look like?
A. Depending on their stage, bed sores can appear as red or discolored skin, blisters, black patches or open wounds.
Q. What is a pressure ulcer?
A. A pressure ulcer, also known as a bed sore, is a wound that forms due to constant pressure or friction on the skin, often from prolonged sitting or lying down.
Q. I have pressure sores on buttocks from sitting too long in one position. What can I do about it?
A. Pressure sores develop due to constant pressure on the skin, leading to tissue damage. Treatment for bed sores on buttocks may include:
- Keeping the area clean
- Changing positions regularly
- Using special cushions
- In severe cases, surgical interventions like debridement or flaps